Fertility Treatments
The first baby born by In Vitro Fertilization (IVF) was named Louise Brown, on July 25th, 1978 in England. Ever since, doctors continued to advance fertility research, leading to the numerous types of assisted reproductive technologies (ART) available today. Couples now face what is often a confusing collection of acronyms when deciding on the best fertility treatment. Learning about these technologies can help couples make more informed decisions.
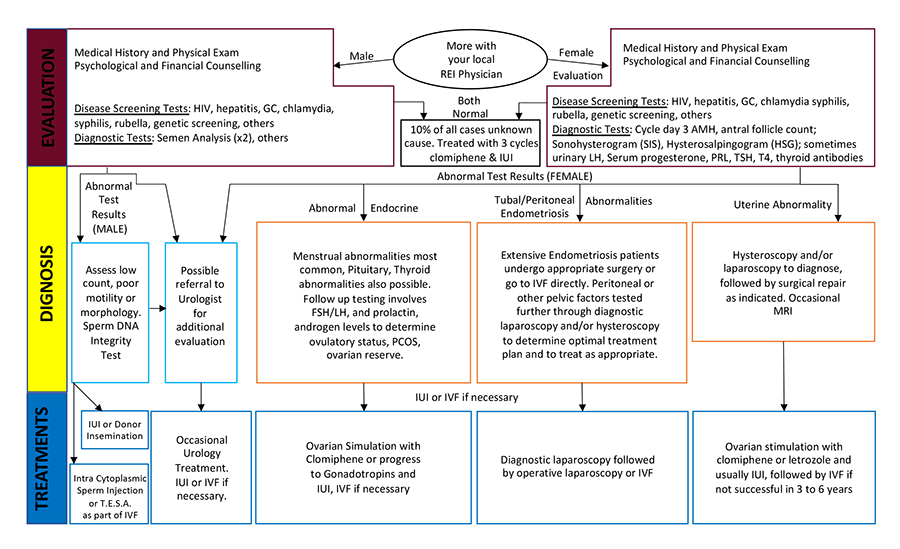
Before Starting Fertility Treatment: Testing and Screening
Before starting an assisted reproductive technology treatment, patients usually undergo a basic infertility evaluation. The evaluation involves a series of tests. It begins with a reproductive endocrinologist (REI), also called a fertility specialist, performing a comprehensive evaluation of both partners. The decision about which tests are appropriate depends on various factors which are unique for each patient. Your fertility specialist can help you decide which tests are appropriate for you. Generally, there are two types of testing the REI performs: screening and specific.
Fertility Treatments – Screening
Screening tests check for general conditions and help protect the patient and the potential child. The conditions doctors screen for can vary among clinics but, generally, screening tests check for:
- Thyroid stimulating hormone (TSH) and Prolactin (PRL)
- Reproductive tract infections before In Vitro Fertilization (IVF) procedures. This often includes testing for chlamydia and gonorrhea, which can cause pelvic infection and tubal damage. These infections can be treated with antibiotics.
- HIV virus and HTLV, which is also necessary to protect laboratory staff working with your sperm or eggs
- Hepatitis B and C, syphilis
- Rubella (German measles) and varicella (chicken pox)
Check with your fertility specialist to learn which tests are required for you.
Fertility Treatments – Specific
Doctors perform specific evaluation tests on women, which can range from simple ovulation calendars to analyzing hormone levels and imaging tests. These specific evaluation tests can include:
- Anti_Muellerian Hormone (AMH), Follicle Stimulating Hormone (FSH), Lutenizing Hormone (LH), Estradiol (E2) and Progesterone (P4).
- Sonohysterogram (SHG): A noninvasive procedure in which an ultrasound is used to check the size and shape of the uterus, and to detect benign lumps of muscle (myomas or fibroids), the uterine lining (endometrium), and ovaries for antral follicle count (AFC) and cysts.
- Hysterosalpingogram (HSG): A radiology procedure that examines the uterus and fallopian tubes. A radio-opaque fluid is injected into the uterus and fallopian tubes and photographed via x-rays to check the uterus for shape, polyps, fibroids (myomas) or scar tissue, and the fallopian tubes for blockage, scarring or other abnormalities.
- Diagnostic Laparoscopy: A minimally invasive surgery in which the doctor examines the internal pelvis and abdominal organs through a small telescope and checks whether the tubes are open. If abnormalities are found they can often be treated at the same time the diagnostic laparoscopy is performed. This is called an operative laparascopy.
- Diagnostic Hysteroscopy: A minimally invasive procedure in which the doctor passes a small telescope through the cervix to examine the uterus, endometrial lining, and fallopian tube openings.
Specific testing for men often includes performing at least two semen analyses which reveals the man’s sperm count, sperm motility and shape. Refer to our Infertility Diagnosis section for more information.
Type of Fertility Treatments
1. In Vitro Fertilization (IVF) is a reproductive technology in which a doctor removes eggs from the ovaries with a small needle passed through the top of the vagina. The extracted eggs are then combined with prepared semen inside the lab – starting the process of fertilization. After this happens, the resulting embryo is placed back into the uterus through a small catheter passed through the cervix.
2. Intra Cytosplasmic Sperm Injection (ICSI) is a procedure in which the doctor injects a single sperm into each egg, using a microscope and sophisticated instruments to perform the procedure. ICSI is performed as part of the IVF treatment cycle. It can increase the chance of fertilization and is often recommended when the male partner has poor sperm quality. In fact, ICSI is a very effective treatment for men who have been diagnosed with male infertility. For males with absolutely no sperm in the ejaculate, sperm can sometimes be surgically retrieved from the testicle or epididymis. Doctors can also perform Donor Insemination (DI), in which donor sperm is placed inside the uterus via a procedure called intrauterine insemination.
Read more about Hysteroscopy and other Infertility Diagnostic and Treatment Modalities here

