Hormonal Therapy
Fertility Drug Therapies for Infertility
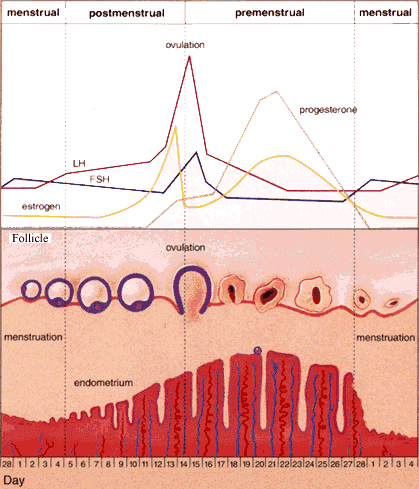
What Is Ovulation?
Ovulation is the process by which a mature follicle bursts and releases an egg. The egg is then picked up by the fallopian tube.
This event marks the transition from the follicular phase of the menstrual cycle into the luteal phase. Controlled ovarian hyperstimulation (COH) is an integral part of many infertility treatments because the development of a single follicle with a good egg, or the development of multiple follicles, improves pregnancy rates. There are numerous ways (protocols) for controlled ovarian hyperstimulation to be carried out. If you have any questions, please feel free to contact ARC, and we will forward your inquiry to an Advanced Reproductive Care physician as geographically close to you as possible. The most widespread protocols involve the use of fertility drugs like Gonadotropins (Follistim, Gonal F, Fertinex, Pergonal, Humegon, Repronex) and Clomiphene Citrate (Clomid, Serophene). The basic steps in these generalized protocols are explained below. As you can tell, generic drug compounds are often referred to by their trade names as well. Before outlining the hormonal treatment for infertility protocols, the table below offers a brief synopsis of the names and types of fertility drugs for women that are most commonly used for controlled ovarian hyperstimulation.
| Drug Generic or Chemical Name | Brand Names | Type of Administration | Function |
|---|---|---|---|
| GnRH agonists (Leuprolide Acetate or Nafarelin Acetate) | Lupron or Synarel | Injection or Nasal Spray | Supress ovaries during IVF, GIFT, or other ART retrieval cycles to prevent premature ovulation prior to egg retrieval. |
| hMG (Human Menopausal Gonadotropins) | Pergonal, Humegon, Repronex | Intramuscular or Subcutaneous Injection | Contain FSH and LH, typically used to stimulate ovaries during ART procedures or for women who do not respond to Clomiphene therapy. |
| FSH (Follicle Stimulating Hormone) | Follistim, Gonal F, Fertinex, | Subcutaneous Injection | Often prescribed for patients who fail to respond to clomiphene or for ART procedures. |
| Clomiphene Citrate | Clomid, Serophene | Oral Tablet | Stimulates ovulation for women with irregular menstrual cycles or to stimulate the development of extra eggs. |
| hCG (Human Chorionic Gonadotropin) | Profasi, Pregnyl | Intramuscular Injection | Often used to simulate LH surge in ART cycles to induce exactly timed ovulation. |
| Progesterone | Progesterone | Intramuscular Injection, or Vaginal Suppository | Often administered during luteal phase of ART cycles or to treat inadequate luteal phase. |
| Bromocriptine, Pesgolide | Parlodel, Permax | Capsule or Tablet | Inhibits prolactin secretion in women with elevated levels.
|
- Clomiphene Citrate (Clomid)
This drug is a competitive inhibitor of estradiol. It blocks estrogen receptors in a part of the brain called the hypothalamus, which causes the hypothalamus to signal the pituitary gland to release more FSH (follicle stimulating hormone) and LH (luteinizing hormone) into the bloodstream. The increased levels of FSH lead to the development of the follicle and egg which secretes more estrogen into the bloodstream. About a week after ingestion of the last clomiphene tablet, the hypothalamus receptors are no longer blocked and thus trigger an LH surge in response to the artificially elevated levels of estrogen in the blood. As you can see from the picture above, the LH surge triggers ovulation approximately 14 days before the end of the cycle (on cycle day 14 in a 28 day cycle, day 21 in a 35 day cycle). If ovulation does not occur as expected, the standard 50mg dosage can be increased based on the discretion of the physician. If pregnancy has not been achieved after increased dosage, the reproductive endocrinologist may recommend adding hCG (human chorionic gonadotropin) to “imitate” the LH surge. As a patient, there are potential side effects to clomiphene therapy that your physician will advise you about- the most common are hot flashes, breast tenderness, and mood swings. The chance for multiple pregnancies during this therapy is approximately 10% for twins and 1% for triplets. Clomiphene is often used as a first treatment to help stimulate ovulatory production. Because of its lower cost, lower multiple pregnancy rate, and its ease of use, clomiphene is often indicated before use of gonadotropins. - Gonadotropins with GnRH agonists
If clomiphene treatment is not successful or if you are preparing to undergo a cycle of ART treatment (e.g. IVF or GIFT), your RE may prescribe gonadotropins that contain both follicle stimulating hormone (FSH) and luteinizing hormone (LH), or FSH alone. Brand names for these drugs include Pergonal, Humegon, and Repronex or recombinant technology produced gonadotropins such as Follistim and Gonal F. Unlike clomiphene treatment, gonadotropins act directly on the ovaries and are often prescribed in order to stimulate the development of multiple eggs during IVF or GIFT cycles. Gonadotropin treatment requires a series of injections and more intensive monitoring than clomiphene and is much more expensive. Most physicians feel that before gonadotropin treatment is started, all other infertility factors should be investigated by a complete infertility study- often including laparoscopy. Multiple pregnancies can occur in approximately 20-40% of gonadotropin induced cycles. Of this percentage about three fourths are twins, while one fourth is triplets or more. Due to the higher risk associated with gonadotropin treatment, patients will receive intensive monitoring and consultation about their options.There are potentially serious side effects– the most significant besides multiple pregnancy is ovarian hyperstimulation syndrome. Although rare, this condition causes the ovaries to be painfully sensitive to pressure due to swelling, and can result in complications that require hospitalization and bed rest. More serious complications can occur, and they should be discussed with your physician before starting gonadotropin treatment.GIFT and IVF procedures regularly utilize gonadotropin therapy to stimulate the ovaries to produce multiple eggs. These eggs are retrieved through a small needle which is placed through the top of the vagina when the woman is under concious sedation anesthesia.This graphic outlines the major steps in gonadotropin treatment as a part of an IVF/GIFT cycle. Oral contraceptives may be given in the month prior to treatment to limit development of small ovarian cysts. Most doctors start gonadotropin treatments on day 2,3 or 4 of the menstrual cycle (where day one is the first day of actual bleeding). The treatment involves a series of subcutaneous injections in the upper leg or buttocks, followed by monitoring of blood estradiol (the most potent estrogen) levels and ultrasound evaluation of follicle development. If satisfactory blood estradiol level and follicle development occur then the physician will trigger ovulation with an injection of hCG (see above). GnRH agonists are prescribed for nearly all patients during gonadotropin therapy for IVF or GIFT to prevent premature ovulation. GnRH agonists such as Lupron and Synarel are synthetic imitators of GnRH which normally stimulates the pituitary gland to produce FSH and LH. However, when a patient is treated with GnRH agonists, the pituitary intially increases its production of FSH and LH, but then stops FSH and LH production due to “downregulation”. Thus GnRH agonists serve to suppress the ovaries and provide the physician with greater control over controlled ovarian hyperstimulation.GnRH agonists can be given starting either in the luteal phase around cycle day 21 as shown above, or in the early follicular phase just after the menstrual period has begun (“flare”). Both protocols prevent premature ovulation. The follicular phase (“flare”) start may occasionally appear to be more effective in women who respond poorly to the gonadotropins. Different investigators have reported varied results with these two treatment protocols, but the luteal phase start (“long suppression”) is much more commonly used.
- Progesterone
Progesterone is the hormone which supports development of the uterine lining (endometrium) in the luteal phase and prepares the endometrium for the embryo to implant. Progesterone supplementation is sometimes used with clomiphene and/or gonadotropins, and almost always used when GnRH agonists are used. Progesterone can be delivered by intramuscular injection or by vaginal suppositories. However vaginal suppositories may not provide adequate blood leves of progesterone. Oral progesterone is also available, but most clinicians feel it does not supply consistently adequate levels of progesterone to the blood stream to be used with ART cycles. - Bromocriptine (Parlodel)
Prolactin is a hormone produced by the pituitary gland that is normally elevated during pregnancy and breast feeding to promote lactation. Sometimes it is elevated in non-pregnant and non-lactating women, which can cause irregular menstrual cycles or inadequate luteal phase. Bromocriptine is a drug designed to lower the levels of prolactin in the blood stream. Bromocriptine is prescribed in cases of elevated prolactin and results in 85-90% ovulatory success rates (where other infertility factors are not present). It is sometimes called by its brand name Parlodel. Another drug with similar action is pergolide, sold as Permax. Your physician may vary the dosage based upon the impact of side effects- the most common of which are drowsiness and nausea. - Corticosteroids
In a few women the adrenal gland may produce excess amounts of androgens, or male type hormones. These increased levels of androgens, such as testosterone and androstenedione, may interfere with normal follicular development and ovulation. In these cases, low doses of corticosteroids can be used to lower the androgen levels to the normal range. One drug commonly used for this is dexamethasone. It is given in an extremely low dose that almost never has serious side effects. - Thyroid
It is important that the thyroid gland function normally for regular ovulation to occur. Simple blood tests can usually detect thyroid problems. In such cases, hormone supplements of thyroid– such as Synthroid or others– may be needed to ensure normal ovulation. Other treatments are sometimes also needed. - Considerations
Some early studies have suggested an increased risk of ovarian cancer following use of clomiphene citrate and possibly gonadotropins, though several more recent studies have not found this association. Definite conclusions await completion of several large ongoing studies. You and your Reproductive Endocrinologist will need to consider and balance the relative risks and benefits involved before undertaking any drug therapy program.
Find Out Which Hormone Treatment Is For You by speaking with a top fertility doctor at one ARC’s member clinics near you.

